Medically necessary diets and intuitive eating.
I originally had this post tacked on to my last post, but decided to separate them. Let’s get right into it!
For some people with certain health conditions (IBS and autoimmune diseases are a couple that come to mind), there are times when following an evidenced-based eating plan does make sense. However, for those who have struggled with restrictive eating or binging (which is typically a side effect of restrictive eating) an eating plan with any level of food restriction isn’t something you can just jump right into. Here’s why I think that doesn’t work…
A few months ago I went to a presentation my friend and mentor Nikki gave where she brought up Ellyn Satter’s Heirarchy of Food Needs. Similar to Maslow’s Hierarchy of Needs, in general, needs on the bottom of the hierarchy need to be satisfied before one can achieve the level above it. Here’s Satter’s Food Needs Hierarchy:
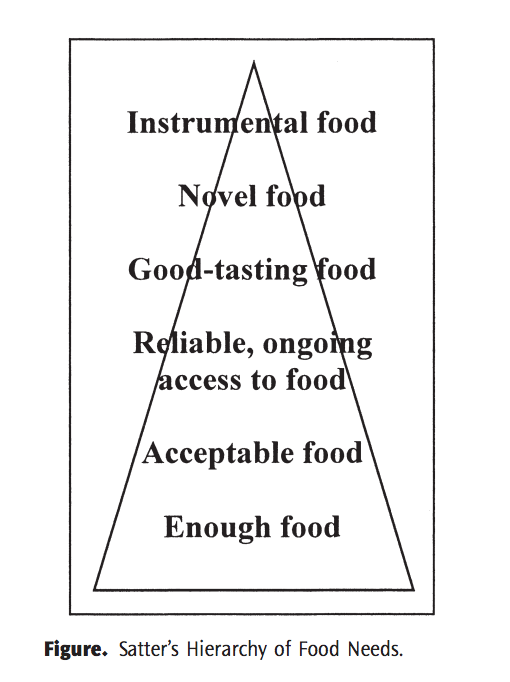
You can read more about Satter’s Hierachy here, but what I want to highlight is that many food interventions given by medical professionals (doctors, physician assistants, dietitians) jump right to instrumental food, when all patients don’t have the skills to be able to follow a medical diet, especially if they live in a diet mentality. To pull in an extreme example from Maslow’s Hierarchy, that’d be like asking someone without shelter and clothing to be relaxed enough to be curious about their personal potential.
Satter talks about instrumental food below:

Some people don’t have complicated pasts with food. They can become gluten free, dairy free, sugar free, FODMAP followers, Wahls follwers, etc. without becoming rigid with their eating and their mental and physical health suffering. But if you’re reading this blog that likely isn’t you. You eliminating food wouldn’t be healthy or wise to do unless you have worked on your relationship with food and it is medically necessary for you to follow a diet that involves avoiding certain foods. And when I say diet here I mean a researched eating plan that has been shown to improve the quality of life for people with particular disease states, not an eating plan that’s sole purpose is weight loss.
Part of the complicated, messy part of being a non-diet dietitian is understanding that for some people eating certain foods does lead to stomachaches, IBS symptoms, autoimmune responses, or other side effects that may be able to be managed with food, but changing one’s food without properly equipping the client with healthy eating behaviors could lead to the client being worse off. If someone is engaging in eating disorder behaviors (i.e. irregular intake, hiding and sneaking food, bingeing, no awareness of hunger and fullness cues, etc.) that part of them needs to be healed before one implements a restrictive nutrition intervention.
Something else I want to briefly mention is….if eating a certain thing doesn’t make you feel good but you continue to give yourself access to it anyways, I believe allowing yourself to have access to that food (and getting the unpleasant side effects) might be an important part of your healing process –part of you working up the Hierarchy of Food Needs– but it’d be best to work with an RD who understands your specific disease state and intuitive eating. I think there is a lot of room for intuitive eating and medical nutrition interventions (aka diets) to be melded together to help clients move up the hierarchy and eat in a way that is nourishing to them. No matter what the disease state, intuitive eating has a place and as my practice continues to grow I know I’m going to want to get clinical supervision from dietitians in different fields to figure out how to support current or former disordered eaters who also have a disease that could benefit from some nutrition intervention.
However, not all people need a medical intervention (aka a diet) to achieve a high level of health. I want to be clear that I am not saying here that the end goal for an intuitive eater should be going on a diet of some sort. I am only saying that for some intuitive eating opens up the ability to follow a medically necessary diet for a disease state they have and allows them to not engage in extreme behaviors (preoccupation with food, bingeing, etc.) as a result of following that diet. Diets are medical interventions that have side effects and before a diet is prescribed it should be considered if someone is mentally healthy enough to follow it.
Lastly, if you have an eating disorder what is necessary to heal that needs to come before any food restriction.
What do you think about this? I’d love to hear from RDs and non-RDs! Have you seen Satter’s Hierarchy of Food Needs before?
If you are an intuitive eater who has to avoid certain foods for health reasons, what’s your experience with that? What did I leave out of this post that I should’ve included?





Very interesting! I really like the language of the hierarchy. I haven’t seen this before but I’ve certainly used the concept even in an acute setting. If a patient has a very poor appetite and inadequate intake, I recommend a liberalized even if their disease state may respond well to a low sodium diet.
With diets that eliminate specific foods (like low FODMAP) I find focusing on what one can eat and celebrating those foods can help to lessen the feelings of restriction. It’s testy waters for sure when mixed with EDs, but not being curled up in a ball due to gas pains after eating can also help there to be less fear of food.
Thanks for sharing, Kate! I always enjoy your thoughtful comments!
Interesting post, Kylie. Ellyn Satter’s work is a guiding force of how I feed my family. As a intuitive eater and someone with an autoimmune disorder, I’ve spent a lot of time thinking about this topic. I’ve realized and have come to accept the fact that I will not eliminate certain foods from my diet in an effort to eliminate symptoms or “heal” my body. My body does best when it has access and freedom to eat all foods in a calm, enjoyable way. During my journey with my autoimmune disorder, I’ve listened to doctor’s advice about eliminating all types of food; dairy, gluten, processed foods, and listened to their speal about why a restrictive “clean” diet would be better for me. I tried it. Luckily however, I’m far enough along in my disordered eating recovery that I could recognize the feelings of what was happening from the restriction and remedied the situation quickly. Plus, my autoimmune symptoms didn’t seem to improve only worsen from the restriction and obsessing so I had faith in trusting my self over doctors opinions. I love good food and I love feeling empowered to choose what I want to eat. That’s what works for me. Others will be different indeed. ?
Thanks for sharing, Amy! I’m glad you recognized what wasn’t working for you and changed things up!
I’m someone with really intense IBS and changed my diet 10 years ago because I was tired of pooping my pants or almost pooping my pants in public, in the car, in school, on runs, etc. It worked. I don’t eat red meat and limit my dairy because both make me feel horrendous and have put me in super awkward situations. I am definitely an intuitive eater but I have a history of disordered eating so balancing these two things became my priority a few years ago. I always make sure if meat is involved I have a tummy alternative so I don’t restrict, but I am someone for whom a diet change has literally changed my life. So I don’t know how I feel about this.
Thanks for sharing, Elizabeth!
Thank you for this post. My husband has Crohn’s disease and 9 years ago we drastically changed our diets in an effort to improve his symptoms. It worked and he has done amazing avoiding certain foods, but it definitely helped me spiral into disordered eating behaviors. It took me a long time to even realize I had a problem because my behaviors seemed so justified, it was like I was on some crazy health crusade. I realized in grad school that I really had a problem and got help (gosh, almost 3 years ago now!). Now I can support my husband in his eating in a way that is healthy and sustainable for him while also not having a meltdown if I eat Kraft cheese at a party or if I decide to eat a cookie. Anyway, I know this is not from the perspective of someone with an autoimmune disease, but caretakers/loved ones of people with these illnesses are also heavily affected by any dietary changes that have to be made. My husband thankfully has no issues with disordered eating whatsoever, he eats so intuitively and recognizes what makes him feel good and what doesn’t. Sometimes he’s willing to “suffer the consequences” and sometimes he knows it’s just not worth it. Either way he moves on with his day. But for me it was definitely a gateway into disordered eating!
Great, great point about caregivers, Ann! I didn’t think about this when writing this post, so I’m glad you brought it up!
I have severe IBS and end up with debilitating pain a majority of days each month. It has been the hardest thing to deal with in my recovery. My dietitian was always clear that we really need to focus on adequacy before the GI stuff. I’ve had slight success with aspects of the FODMAP diet. I will say, I’ve solidly been in full-on recovery for a year and things are finally starting to feel easier. Being flexible with food; making choices that sound good and probably won’t hurt my guts; eating food that sounds great and may hurt my gut, and it’s worth it! My dietitian and I have been having this discussion a lot and it’s a tough line to walk. Good things to think about, for sure.
Thanks for sharing your experience, Hillary! Did you see this post by Rachael? https://www.rachaelhartleynutrition.com/blog/intuitive-eating-and-ibs-part-2 I thought she did a great job talking about IBS.
I love this. It definitely took me a long time to be able to comfortably balance foods that make me feel terrible with better choices for me based off of my personal needs. I had a major surgery 10 years ago that affected my organs/digestion so certain foods are very difficult for my body and can cause me a lot of pain/discomfort… but I had to let myself feel terrible and eat the foods anyway to legitimately stop wanting to eat them. Having said that I still eat them sometimes when I want them, but I do my best to keep portions small enough to not cause pain… or I just deal with it because it feels worth it the odd time.
Thanks for sharing, Amanda!
It is definitely tricky to navigate. Modifying my diet has been a lifeline for me as I’ve dealt with several autoimmune issues. At one point I was covered head to toe in psoriasis and feeling SO desperate. But it has had it’s share of mental struggle. Working with a Dr. and a therapist has been really important. But I’ve appreciated the parts of life I’ve gotten back through diet changes. Since I’ve been pregnant or nursing the last 4 years my conventional treatment options were limited. People ask me how I can eat this diet and how I’m so “good” and it makes me mad. Like, if it didn’t make me ache like a 90 yr old and break out in itchy rashes you bet I wouldn’t be “good”. I have gotten a lot better about not being afraid of the treats I can have or worrying about every single time I don’t feel well. Often it’s more stress than food. So I enjoy my chocolate and coconut milk ice cream when I need it for my mental health but I can actually leave it in the freezer and realize I don’t feel like eating it sometimes. I never would have believed that it was a possibility years ago in the thick of disordered eating. I think, having traveled down this path that I really hesitate to recommend anyone change their diet if they don’t have to. It’s so hard to stay mentally healthy on a medical diet :/
Agreed, Annelise! Medical diets should only be started if medically necessary and any disordered eating/ED symptoms are being addresses simultaneously or prior. THANK YOU FOR SHARING A BIT OF YOUR STORY!
I think the thing that is ironic is that I actually didn’t make changes that could have been so helpful early on (like more fat, regular meals, stress management, REDUCE EXERCISE (!!!) because of my disordered eating habits. The dietary modifications really were only helpful once I was willing to actually eat enough food (which btw now looks like a ton of fat and frying plantains for breakfast ?) and had some coping strategies for the things my ED was helping with. It’s still messy, but I don’t feel like I “can’t” eat things, just that I don’t want to because I don’t enjoy feeling ill.
This reply and your original comment speak right to me, Annelise. Especially the part about “The dietary modifications really were only helpful once I was willing to actually eat enough food.” Spot on for me and something I am just beginning to navigate. Thank you so, so much for sharing. Truly.
I have never seen Satter’s hierarchy before. I think I’m going to print it off to put on my desk in my office. I work as a dietitian where many of my patients are diabetics and many struggle financially. This is helpful in remembering that I can’t jump in always telling them how control carbs at each meal and regular meals if they aren’t even in a place of getting regular meals. I do food demos at a food distribution center, and while we do try to make balanced meals with healthier alternatives, my focus is showing them how to use all foods they are provided with in order to meet the most basic need of having food. It made me realize that sometimes the healthiest thing for us all is not any specific eating plan but just being able to regularly eat a variety of foods. Thanks for sharing.
“It made me realize that sometimes the healthiest thing for us all is not any specific eating plan but just being able to regularly eat a variety of foods.” –> yes yes yes. I so agree!
I struggled with eating disorders most of my life, entered a strong recovery and remission, and then got hit with a number of medical issues and autoimmune disease. I have found it so so difficult to eat in a way that is good for my body because any time I feel that I have to deprive myself, I panic. I hope that when my health is more stable, I can go back to my HAES dietitian (who I adore) and find a way to balance a way of eating that may improve my symptoms where I don’t feel deprived or feel the need to eat everything I “Can’t have”. In fact, I’ve realized I just can’t label any foods as “can’t haves” or I feel absolutely insane! I am so glad that the intuitive eating dietitians have been talking about this issue. Thank you.
I agree it’s good the intuitive eating community is talking about this; AND am also hoping dietitians in other fields look into how helping a client have a normal relationship with food could be integral to their work with clients within the population they are an expert in. I’ve had a few clients referred to me by holistic nutrition and functional medicine dietitians in Houston and think it’s awesome. Those dietitians are highly trained in their field and are able to recognize when the client needs more support than they can provide and they need to refer out to someone trained in intuitive eating/EDs to help the client get to a place where diet changes that improve health can be made.
I really like this post! An important of the piece of the conversation is that eating disorder symptoms can often mask as digestive symptoms because they can wreck your gut and hormones for sure. A lot of people who restrict their diet will probably have some other symptom, whether it’s gut pain, headaches, period problems, etc. that won’t be fixed by a FODMAPS diet, but rather eating more.
It’s easy to convince yourself when you’re too thin that the problem isn’t the under eating, but instead some other problem that could be fixed. It’s way too easy to jump on this eating disorder if you will than fix the actual problem.
My mom suffers from T1D/insulin abuse (which is a REALLY shitty type of eating disorder) and frequently justifies harsh diet shifts in the context of “healing” even though it just makes her more restrictive so I wish I could get her to understand this. This gives me a lot to think about.
Thanks for sharing, Savannah! All good points. I’ve been working on a diabulimia post for way too long now…hopefully it’ll get posted by the end of the year.
I am a type 1 diabetic who went through years of diabulimia in college and it almost killed me. Ten years out of college and I am finally an intuitive water but there is always that fine line of managing the carbohydrates I eat to keep my blood sugars steady and honoring my actual cravings for what I want to eat. While my blood sugars may be slightly easier to control with a very low carb diet, my mental health greatly suffers for it, so I have worked hard to find ways to be able to eat carb heavy foods (cookies, pizza, pasta) while keeping my A1c in the fives. I have a great IE dietician/certified diabetes educator (CDE) who I see monthly to help keep me on track because while the IE journey has been so enlightening and life affirming for me, it is certainly a lot of hard work with a relentless autoimmune disease!
So glad you found an IE + CDE dietitian to support you in this, Meaghan! That’d be a tough path to walk alone!
Meghan- I am sorry that you suffered with Dia-bulimia for so long and I am so glad that you have help now and a therapist to talk to. Sending love your way. I’m glad that you’ve been able to find balance in treats and such- I’m sorry that the nature of diabetes means you can’t just eat what you want and let your body “figure it out” like I have the privilege to.
I hope that my mom can come to the same conclusion as you- that it’s actually better for her to eat everything and just account for it all with insulin. Her mental health is poor. With the technology that’s around today, measuring blood sugar and giving the appropriate amount of insulin has never been easier.
Proud of you <3
I love that you addressed this, because it is something I really stress a lot in my recipes/articles.
First of all, it is so frustrating that “diet” is so deeply linked to weight loss. I talk a lot about following different diets – that is, eating plans that dictate that some foods may not be feasible for health reasons – and I cringe every time someone tells me that they want to follow the diet to lose weight. That’s not what it’s about. There is no non-clunky word for diet that isn’t deeply intertwined with weight loss, and that really bothers me.
But I also cringe similarly when people dismiss all elimination diets as “disordered”.
I’m not saying that there isn’t a link for some people, of course, but the truth is that I’ve never worried less about what I ate since I figured out what exactly made me sick.
Before that I was afraid to eat almost anything out of my usual routine and it was frustrating and unpleasant – impossible to enjoy food.
Once you (Well, I) identify the medically necessary ingredients to eliminate, it is possible to have a positive relationship with food again!
There is such a STRONG belief that health is solely determined by a narrowly defined body size. I agree it’d be nice if the word “diet” wasn’t so deeply linked to weight loss, but until fat is less feared I think it’s unlikely to happen.
I’m glad finding specific things that made you feel sick improved your relationship with food! I think my fear for some people is that when they can’t find what food makes them feel sick (because it’s actually anxiety) they eliminate more and more and more. Everyone is different.
Thanks for sharing, Nora! It was fun seeing your name pop up in the comments again!
I follow a low carb, sugar free, high fat diet due to blood sugar issues, as well as depression and (potentially autoimmune) hypothyroidism. At first, I would allow myself to have sugar and carbs on occasion, even though it made me feel awful, until it finally clicked for me that this is how I want to eat to feel my best. Now I don’t want or crave sugar anymore. I think another thing I would add is that such diets don’t have to mean depriving oneself of delicious food either. I have found an amazing pizza recipe that even carb lovers can enjoy, have learned to love bacon, and even get to have dark chocolate, unsweetened peanut butter, and sugar free, high fat ice cream that tastes as good or better than the real thing! I thought this was a restrictive “diet” at first but now it’s just habit, how I eat for health, and I’ve I found that mindset makes all the difference. :)
I’m glad you have found what has worked for your physical and mental health! Thanks for sharing, Kaylyn!
For anyone reading the comments…this is the diet that worked for her. You following a low carb, sugar free, high fat diet may lead to obsessive thoughts about food or out of control eating and may not be an appropriate option for you based on your values, your history/relationship with food and what you want your life to look like.
Great post! And very timely for me. I was just diagnosed with gestational diabetes just when I was really starting intuitive eating. What doesn’t apply from your post is that if I have treats that spike my blood sugar, it hurts my baby–not me! In a way it’s both more motivating to not cheat the diet but also less motivating in the moment when temptation is very strong because I can’t actually see or physically feel the damage it may be doing. It’s been emotional so far because as I check my sugars 4 times a day, I get a very immediate pass or fail many times. If I really enjoy a food that would otherwise be healthy except for a diabetic, but my numbers are too high, it’s so defeating. Eating can easily feel like an actual battle or test instead of a culinary and social experience. Hopefully it’s just a season for me and I’ll be able to go back to normal after, but it’s a struggle. Mama wants a bowl of cereal…
Hey Ashley, Thanks for sharing!
It’s a bummer when eating gets more complicated. I wonder if cereal was paired with a protein + fat source, like eggs, if your blood sugar could stay in a healthy range. Or maybe cereal for a snack with a cheese stick or something for protein/fat, instead of first thing in the morning, could be an option?
Just throwing out some ideas…you may have already tried all this! You know your body best.
I struggle with a lot of digestive issues and I’m not sure what is causing them, whether it be food, stress, or gut imbalances. I think the hardest thing for me is craving treats, but knowing if I eat them I usually feel pretty poorly, so I try to refrain, but then eventually end up going overboard because I restricted myself for so long, and then of course I feel even worse and it starts all over again. It’s definitely a vicious cycle!
Have you tried incorporating a treat after every meal? Sometimes it’s the amount that can make one feel crappy, but consistently letting yourself have something sweet can help you not go overboard. Nothing amplifies a craving for sweets like restriction!
Hey Kylie! I found this article and your blog while researching about intuitive eating with a food allergy. I am a vegetarian for ethical reasons, and my diet is largely plant based (if you count TJ’s yogurt or cereal as plants ? haha) and I eat a lot of nuts, seed butters, vegetables, TONS of TONS of fruit and grains (processed ones, haha— pasta, whole wheat tortilla wraps).
But I do have an allergy to dairy. While i was struggling with disordered eating, I used my allergy as an excuse to stay away from pizza, Mac and cheese…. now I just pop a pill & enjoy my ziti + spinach salad (yesterday’s lun)
Thanks for all your knowledgeable insights, delicious recipes and sunny personality!
Another relevant post! I was diagnosed with gestational diabetes and am supposed to be following a lower carb diet. Luckily, the way I intuitively eat isn’t super carb heavy and I haven’t changed much and my blood sugar numbers have been fine. Loving exercise helps. That being said, it’s absolutely fascinating that even with a slight carb restriction, it is made extremely clear that our body NEEDS carbs to function and in fact, I should be making an effort to be eating carbs regularly to keep blood sugar at a good level. Just an interesting observation since we so often hear “carbs are the devil” (I legit had a doc say that to me).
“I should be making an effort to be eating carbs regularly to keep blood sugar at a good level” <--YES!! Having carbs consistently throughout the day (rather than restricting and then ending up desperately needing carbs because blood sugar gets too low and then having body crave ALL THE CARBS to get blood sugar back to a good range) is a way better options for helping out your blood sugar!
This is very timely. I am an intuitive eater who has recovered from an ED, and am now realizing that dairy and possibly gluten make my stomach very unhappy. I don’t have a diagnosis, but I’m exploring things myself. It’s bee tough to navigate intuitive eating with this discovery because for so long I said that all food was okay and people shouldn’t restrict certain foods unless medically necessary, but now I’m realizing I need to make a change. I am trying to keep normal food around (i.e. homemade gluten free cookies) so I don’t feel deprived.
I am so happy that you wrote this post. Mostly because having certain conditions (hypothyroidism and ibs) makes intuitive eating a little bit harder to navigate. I love the freedom that comes with intuitive eating but I feel like I’m always second guessing myself with what I should really be eating. This graph makes everything a little bit easier to understand. I have learned that using evidence based diets is so important because there are a million and one diets out there that claim to fix everything. Are there actually any eveidence based diets that help autoimmune disorders like Hashimoto’s thyroiditis? Not that I’m there yet but would love to know! Thanks Kylie!
Pingback: 5 Thoughts [thoughts on hawaii and a helpful body image analogy] - The Real Life RD
THIS IS GOLD.
I have to avoid gluten. In my restrictive eating days, we would go to a restaurant that had gluten-free buns and I would still not get them because I already had my starch (fries).. what a sad life. Now I am so excited when restaurants are so accomodating! BUT also.. sad when they are not. I have learned what restaurants are good about accomodating and ones that are not. It’s not fun to eat unsatisfying foods. I don’t go to the restaurants that are not accomodating.
Agreed that it’s not fun to eat unsatisfying foods!
I love this!
I have a passion for teaching people how to have a positive relationship with food and their bodies and have adapted the intuitive eating mindset myself over the last year. I am also very much interested in possibly working in the critical care setting in hospitals. You mentioned that intuitive eating can be combined with medical nutrition interventions. How would you say is the best way to approach this? As a diet tech at a local hospital I always struggle with educating patients for CHF and low sodium/fat diets because I don’t like telling people to reduce/restrict this in their diets but this also classifies as medical nutrition intervention so how do you go about combining that with intuitive eating? TIA!
Also interested in the answer here, as I work on a CHF floor as a nurse!
This was/is exactly me. Throughout college I started restricting foods more and more in a quest for the “perfect” diet and overexercising so I could stay thin. Once I graduated, I started having some severe digestion issues. I was diagnosed with ulcerative colitis and tried traditional medicines, but nothing helped. Then I went to functional medicine and it made my fears of foods so much worse than they already were. I was literally told how EVERY SINGLE FOOD is bad for me: grains-inflammatory, veggies-too much fiber and sometimes sugar (ugh how sad this makes me that I was told vegetables are bad and believed it!), fruits-too much sugar, meat- too hard to digest, dairy-was already lactose intolerant, beans-inflammatory, nuts and seeds-too difficult to digest. At one point I was eating bone broth and pureed cauliflower soup and that was it. The stress and fear for all foods it brought me was terrible and I’m still trying to climb out of it 4 years later. When you have a doctor telling you all these things and you are so desperate to feel better, you’re willing to do a lot of things. I’m so glad I can now look back and see how wrong that was and know that moving on from those approaches was the right decision. I still am no better health wise, but at least some of the stress around food has begun to faed away and that is making a big difference.
Hi! I have been practicing intuitive eating since about August, and since have also been diagnosed with IBS. Interestingly enough, once I stopped restricting foods in hopes to identify my triggers, my IBS symptoms/episodes decreased dramatically. I think a lot of my symptoms were related to stress and anxiety around eating. I have a lot less stress/anxiety around food now, but I still have some episodes. I havent started any diets yet because i already feel that my symptoms are much more manageable since moving to intuitive eating, and I’m just enjoying eating all the foods!
Yes, Morgan! Thanks for sharing! Anxiety over food can be the root or a huge part of IBS symptoms for some…when the mind is actually what is having trouble processing the food, not the body.
I’m late to comment but I enjoyed this article a lot. I’ve been aware of Ellyn Satter’s hierarchy of needs for quite some time, not sure when I was first introduced. I find there is nearly zero resources out there for general MNT and intuitive eating principles despite the very clear need in the growing dietetics field. I’m a full time inpatient RD and am frequently consulted to educate 80 year olds on heart failure to limit sodium (never mind they are underweight and haven’t had salt since Reagan was in office) or diabetes/renal education for people who live off food stamps and don’t even have reliable access to groceries. It’s bad practice and I feel unethical to pretend like everyone can be treated the same way.
Thanks for the comment, Melissa!
Pingback: Basic Body Confidence: What It is and Four Mindsets and Practices that Develop It – Love Is Stronger
I stumbled across this after recently being diagnosed with both Rheumatoid Arthritis and Crohn’s and I also have a history of eating disorders. I have seen dozens of specialists and medical providers, and none are educated or trained in HAES or intuitive eating. One even laughed at the concept. I continue to be amazed and dismayed at all of the medical providers who say they are providing care but continue to push things like BMI and restriction-based diets that have no foundations in medical science or evidence based research. I am exhausted from advocating for myself in doctors’ offices and trying to educate them on what they should already be doing. I have been working with a HAES and Intuitive Eating certified RD for over a year, and we constantly find that healing my relationship with my body and food is more effective than any restriction diet or “wellness plan”. The American medical system is doing harm to patients daily and it needs a huge overhaul in this area!
Pingback: Noticing when your food insecurity is being aggravated. – Yeah…Immaeatthat
Pingback: Noticing when your food insecurity is being aggravated. – immaEATthat